PREGNANCY
Breech Baby? What to Know About External Cephalic Version
If your baby is breech, you may be contemplating an ECV.

Written by
Happiest Baby Staff
Around 3% to 4% of full-term pregnancies involve a breech baby, meaning their bottom or feet are pointing down instead of their head. If that's your situation, you've probably already started down many internet rabbit holes. But before you spiral, know that you do have options, and one of your most well-studied among them is a procedure called external cephalic version, or ECV. Here's what it involves, when it's done, and what to consider.
What does it mean if my baby is breech?
A breech presentation means your nugget is positioned with their booty, feet, or both aimed toward the birth canal, rather than their head.
There are a few different types of breech presentation:
Frank breech (bottom down, legs up by the head)
Complete breech (sitting cross-legged)
Footling breech (one or both feet pointing down)
Your little one’s position matters because a head-down (vertex) position is considered the safest for a vaginal delivery. When a baby is breech, delivery can be more complicated—the body comes out first, and the head, which is the largest part, is delivered last. This can increase the risk of issues like cord prolapse or the head getting trapped. For these reasons, the vast majority of breech babies in the United States are delivered by c-section.
What is an external cephalic version?
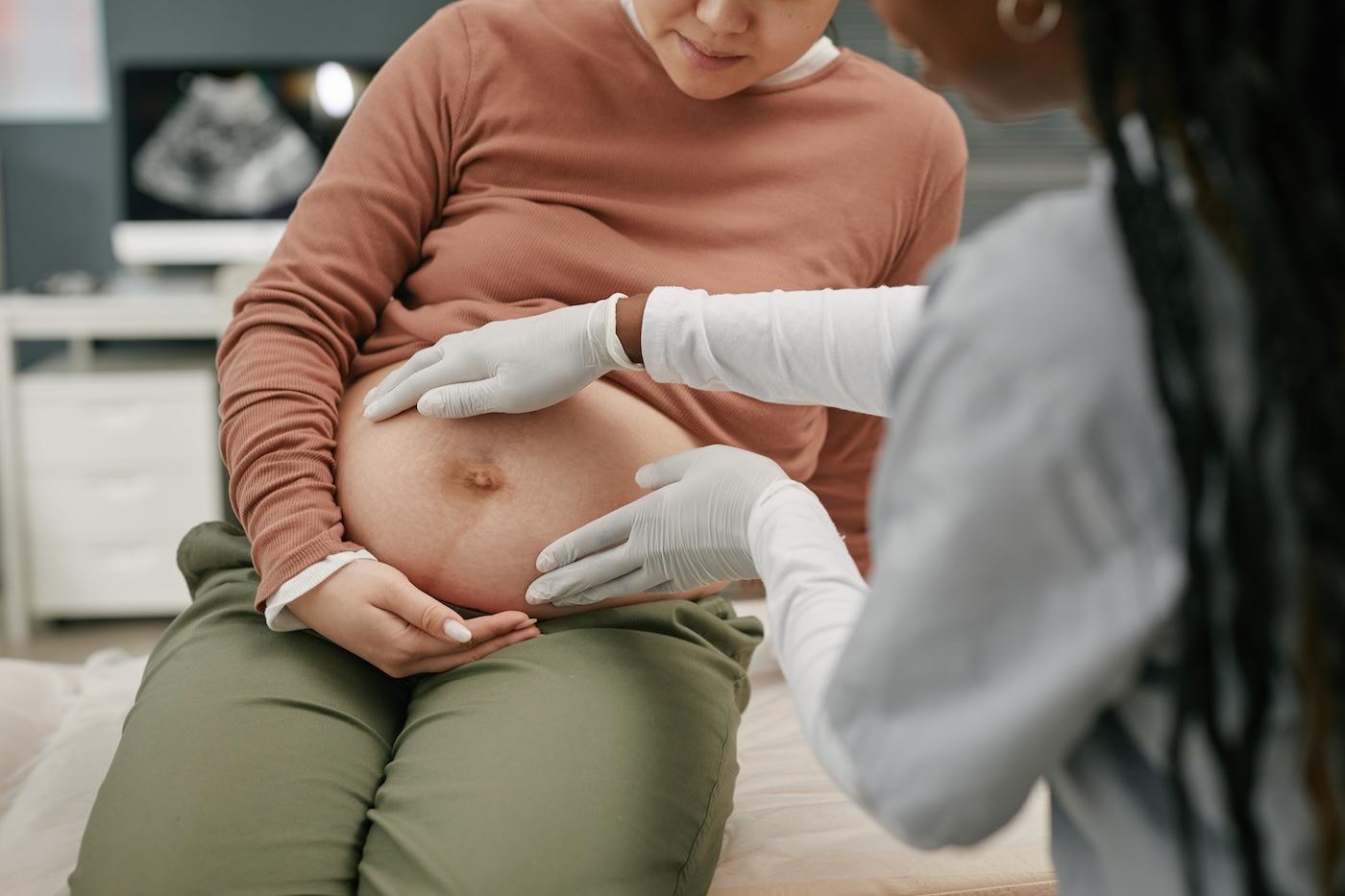
An external cephalic version (ECV) is a procedure in which a healthcare provider uses their hands on the outside of your abdomen to gently rotate your baby from a breech position to a head-down position. The goal is to increase your chances of having a vaginal birth and to help avoid an unnecessary c-section. The American College of Obstetricians and Gynecologists (ACOG) recommends that all pregnant people near term with a breech presentation should be offered ECV, as long as there are no complications that would make this risky.
When can I have an ECV?
Typically, an ECV is performed starting at 37 weeks of pregnancy. There are a few reasons for this timing:
If your baby is going to turn on their own, it's likely to happen before 37 weeks.
Performing ECV at 37 weeks or later reduces the chance that the baby will flip back to breech after a successful turn.
If any complications arise during the procedure, your baby is considered early term and can be safely delivered.
Your provider should begin checking and jotting down your baby's position starting at 36 weeks so there's time to plan for an ECV if needed.
Does ECV work for all breech babies?
Not all breech babies can be turned, and ECV isn’t a good fit for everyone. The overall success rate is around 50% to 58%, but it varies widely depending on factors like the experience of the practitioner, whether you've given birth before, the amount of amniotic fluid, and the position of the placenta. People who have had a previous vaginal delivery tend to have higher success rates than those in their first pregnancy.
There are certain issues that make an ECV a little risky, so they likely won’t offer it if you have:
Nonreassuring fetal heart rate
Multiple pregnancies with a breech-presenting fetus
Very low amniotic fluid
Significant fetal growth restriction
If you've had a prior c-section, ECV may still be an option—but your provider will evaluate your individual situation carefully.
Where is an ECV performed?
ECV is performed in a hospital setting—usually in or near a labor and delivery unit—where c-sections are immediately available, as a safety precaution. While complications are rare, having an operating room nearby means your care team can respond quickly if an emergency c-section becomes necessary.
What happens during an ECV?
Before the procedure, your provider will use ultrasound to confirm your baby's position and check your amniotic fluid levels. They’ll likely hook you up to a fetal heart rate monitor (a nonstress test) to keep tabs on your baby. You'll likely be asked not hold off on eating beforehand, just in case you need a c-section.
To help relax your uterus and make the procedure easier, you may get a tocolytic medication (such as terbutaline), which temporarily reduces contractions. Some providers also use regional anesthesia—like a spinal or epidural—which research shows can increase ECV success rates.
During the ECV itself, your provider places their hands on your belly and applies firm, steady pressure to guide your baby into a forward or backward somersault. The actual turning often takes just a few minutes, though the total visit—including monitoring before and after—can take around two hours. You may feel discomfort or pressure during the procedure, but your provider will stop if you’re in a lot of pain or if your baby's heart rate changes.
Afterward, they’ll keep an eye on your baby's heart rate. If you are Rh-negative, you'll receive a dose of Rh immunoglobulin. If the ECV is successful, you can typically go home and continue with your regular prenatal care.
What are the risks of an ECV?
Serious complications from ECV are unusual. The most frequently reported issue is a temporary change in the baby's heart rate during the procedure, which usually resolves once the procedure ends.
In rare cases (less than 1% each), risks include:
Placental abruption
Umbilical cord prolapse
Premature rupture of membranes
Fetal-maternal hemorrhage
Stillbirth (very rare!)
The rate of emergency c-section within 24 hours of ECV is around 0.5%.
A Cochrane systematic review found no differences in Apgar scores, umbilical cord pH, or neonatal deaths between babies who underwent ECV and those who did not—reinforcing that the procedure is generally safe when performed by an experienced provider in an appropriate setting.
What happens if the ECV doesn't work?
If the ECV is unsuccessful, your provider may suggest trying again on a different day—sometimes a second attempt succeeds, especially with the use of regional anesthesia or tocolytic medication. It's also worth knowing that about 3% to 7% of breech babies will spontaneously turn to a head-down position on their own, even after a failed ECV.
If your baby stays breech, the most common next step is a planned c-section, typically scheduled around 39 weeks. In some cases, a vaginal breech delivery may be an option, but this really depends on your doctor’s experience and your hospital's protocols.
After a successful ECV, there is a small chance (around 3% to 5%) that your baby may flip back to breech, so your provider will continue to keep an eye on your baby's position at prenatal appointments.
Is there anything else I can do to make my breech baby turn?
You may have heard of other ways to encourage a breech baby to flip. Some of these approaches include:
Tilted positioning (postural management): Techniques like lying on your back with your hips elevated (sometimes called a "breech tilt") have been used for decades, but a Cochrane review found insufficient evidence to confirm their effectiveness.
Moxibustion: This traditional Chinese medicine technique involves burning an herb (mugwort) near a specific acupuncture point on the little toe. An updated Cochrane reviewfound moderate-quality evidence that moxibustion plus usual care may reduce the number of breech presentations at birth, though it did not significantly reduce the c-section rate. If you're interested in trying it, chat it with your doctor!
Chiropractic care (Webster Technique): Some pregnant people seek chiropractic adjustments designed to balance the pelvis and relax surrounding ligaments. While there is anecdotal support, high-quality clinical trial data is limited.
None of these approaches has as strong an evidence base as ECV, and none should be used as a substitute for discussing your options with your healthcare provider. The bottom line: If your baby is breech at 36 weeks or beyond, talk with your provider about whether ECV is right for you. It's a well-studied, relatively low-risk procedure that could help you avoid a c-section—and that conversation is always worth having.
More on Pregnancy:
- What Is a Membrane Sweep—and Do I Really Need One?
- What Happens During a Labor Induction?
- Tips for an Easier Labor and Delivery
- The Causes of Preterm Labor
- What to Know About Pain Relief During Labor
***
REFERENCEAmerican College of Obstetricians and Gynecologists: If Your Baby Is BreechMode of Term Singleton Breech Delivery: ACOG Committee Opinion No. 745, Obstetrics and Gynecology, Aug 2018Cleveland Clinic: External Cephalic Version (ECV)External Cephalic Version: ACOG Practice Bulletin No. 22, Obstetrics and Gynecology, May 2020External Cephalic Version for Breech Presentation at Term, Cochrane Database of Systematic Reviews, Apr 2015Reviving External Cephalic Version: A Review of Its Efficacy, Safety, and Technical Aspects, Obstetrics & Gynecology Science, Oct 2019Prisma Health Academics: External Cephalic Version (ECV) Clinical Practice GuidelineAmerican Society of Anesthesiologists: Statement on Anesthesia Management and Support for External Cephalic VersionExternal Cephalic Version for Breech Presentation at Term, Cochrane Database of Systematic Reviews, Apr 2015Cephalic Version by Moxibustion for Breech Presentation, Cochrane Database of Systematic Reviews, May 2023External Cephalic Version for Breech Presentation Before Term, Cochrane Database of Systematic Reviews, Jul 2015Disclaimer: The information on our site is NOT medical advice for any specific person or condition. It is only meant as general information. If you have any medical questions and concerns about your child or yourself, please contact your health provider.
SHARE THIS ARTICLE
MOST LOVED
Sleepytime Sidekicks












