PREGNANCY
11 Things Your Embryologist Wish You Knew About IVF
If you’re considering IVF, chances are you have a lot of questions. Here, some much-needed answers.

Written by
Happiest Baby Staff
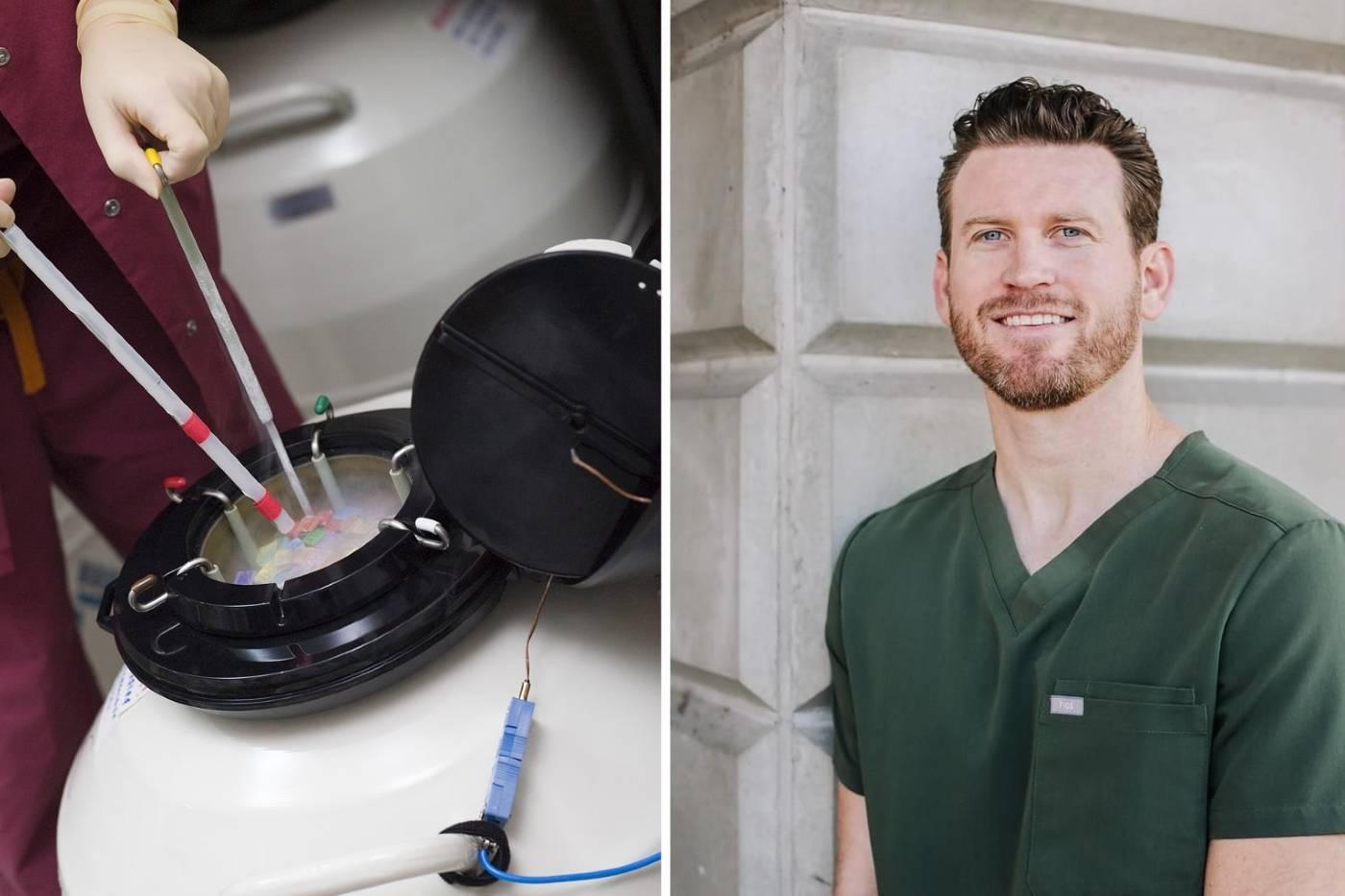
A recent Pew Research Center report found that 42% of Americans have either had fertility treatments or know someone who has—and that number just keeps on growing. In fact, a 2022 report in the journal Reproductive Sciences speculates that, in the near future, as many as 10% of all children will be conceived through IVF in many parts of the world. But even with IVF’s growing popularity, there’s still a lot of confusion and, frankly, misinformation. That’s why Happiest Baby asked Shaun Reed, an embryologist at Utah Fertility Center (who you may recognize from his viral TikTok and Instagram videos), to help clear up some of the biggest questions you might have about IVF and embryos. Here, 11 things this embryologist wants you to know about IVF.
#1: No, an embryo is not a baby!
“Zygotes and blastocyst embryos are just one stage of development on a long list of steps before becoming a baby,” says Reed. Here’s a mini bio lesson: When an egg is fertilized it becomes a zygote, which is a single cell with genes from both parents. The zygote continuously divides, eventually forming a ball of cells called the blastocyst. About 12 days after fertilization, the blastocyst then develops into an embryo. It remains an embryo for about nine weeks before becoming a fetus.
And becoming a baby is never guaranteed. “The fertilized egg, or zygote, is estimated to have a 40 to 75% failure rate to implant and result in a live birth,” says Reed. “Blastocyst embryos have about a 40 to 60% chance of implanting.” For those dealing with infertility, these odds are worse.
“To call a zygote or blastocyst embryo a ‘person’ is not only a mislabel, but it also disrespects the way nature works and is harmful propaganda used to reduce autonomy of people needing IVF treatment,” says Reed.
#2: Frozen embryos don’t expire.
“As far as we know, frozen eggs and embryos have no expiration date,” says Reed. “They are frozen in liquid nitrogen, which is super cold at -320 degrees Fahrenheit. In fact, it’s so cold that frozen eggs and embryos are essentially frozen in time when it comes to aging. There is no reason to worry about how long your eggs or embryos have been frozen.”
#3: It’s easier to freeze embryos than eggs.
“Easier” doesn’t always mean it’s the best choice for you, however. “Freezing eggs is a little more tricky than freezing embryos, because eggs are a bit more sensitive to the freezing and thawing process,” says Reed. When freezing embryos, the eggs are fertilized and then grow for five to six days until they reach the blastocyst stage. “On top of that, you won’t know how many of your eggs will develop into viable embryos until after they’re thawed and inseminated.” On the other hand, embryos tolerate freezing and thawing better—and you can rest assured that they’ve made it to the blastocyst stage of development.
#4: Abnormal embryos are common.
Embryologists do what’s called Preimplantation Genetic Testing (PGT) on embryos, where they biopsy a couple of cells from each embryo to see if there are two copies of each chromosome. “A certain percentage of embryos will have either extra or missing chromosomes, which is called aneuploidy,” says Reed. “These embryos will either fail to implant or miscarry very early on.” The percentage of embryos that come back normal can really vary from person to person. That said, “aneuploid rates are fairly age dependent, which means, as the age of the female goes up, so does the rate of abnormal embryos,” says Reed, who estimates that 40 to 70% of embryos come back normal—and 30 to 60% come back abnormal.
#5: Embryo grading is subjective.
“Embryo grading can be a bit of a loaded topic,” says Reed. “Each embryo is unique-looking, and each embryo can be graded slightly differently depending on which embryologist is grading it.”
Essentially, there are three main things embryologists are looking at when grading an embryo: expansion, inner cell mass, and trophectoderm. Here’s what that means:
- Expansion: On day five of development, the embryo forms a fluid-filled blastocoel cavity in the middle. This is the “blastocyst” stage of development. Here, embryologists use numbers 1 through 6 to indicate the level of expansion of the embryo. “A fully expanded blastocyst is a 4; hatching out of its shell is a 5; and a fully hatched embryo is a 6. Anything below a 4 is called an early blastocyst,” says Reed.
- Inner cell mass (ICM): The ICM is a clump of cells that have come together along the perimeter of the embryo. This ball is made up of pluripotent stem cells that’ll develop into the actual fetus after implanting in the uterus. “The ICM gets a letter grade of A, B, or C, with A being the best. We are simply looking at the size of the ICM and level of compaction of the cells,” says Reed.
- Trophectoderm: These are the cells (usually a few hundred) around the perimeter of the embryo. These cells hatch and implant in the uterus, developing into the placenta. “These also get letter grades of A, B, or C. When grading, we are looking at the number of cells in the trophectoderm and their level of uniformity,” says Reed.
#6: Lower grade embryos can still be viable.
“While the data show a slight trend toward higher-graded embryos having better success, it’s important to remember that ‘lower’ grade embryos also make beautiful babies at a very good rate,” says Reed. “Don’t get discouraged if your best-graded embryo isn’t an AA.”
#7: Infertility is not just a female problem!
Of the roughly 15% of couples in America who have trouble conceiving, over 50% of the time, there’s a male infertility issue. “One huge problem is that many cases of male-factor infertility are overlooked,” says Reed. “A fertility doctor will have the male patient do a semen analysis at initial consultation, and as long as it looks mostly good, they will never take a closer look at the male partner again.” Reed speculates that this is partially because fertility doctors, known as reproductive endocrinologists, receive “little-to-no training in male reproduction.”
#8: Assisted hatching is not for everyone.
“Assisted hatching is where we use a laser connected to a microscope to punch a hole in the shell of the embryo,” says Reed. “The thought is that the shell of the embryo is a bit stiffer after being frozen and thawed.” Many labs routinely hatch after thawing an embryo and before transfer, so the embryo has an easier chance of getting out and implanting in the uterus.
But the thing is, “data doesn’t show a strong positive impact of hatching on outcomes, but they also don’t show a negative impact,” says Reed. “While many labs still do it in case it helps, but if your lab doesn’t hatch, I wouldn’t stress it at all.”
#9: You can’t create embryos of a certain sex.
“When people ask me to try to make them embryos of a specific [sex], I tell them I’m so good that I’ll be able to do that for them with about 50% accuracy!” says Reed. “The point being, we can’t create embryos to be a specific [sex]. To do that, we would have to be able to tell the difference between male sperm and female sperm…but they look the same!” That said, embryologists can transfer embryos of the sex that you want.
#10: You can’t create identical twins, either!
Identical (monozygotic) twins come from one embryo splitting in two. “We can’t intentionally cause this to happen with IVF,” says Reed. “Patients could transfer two embryos and if they both stick, then they would have fraternal (dizygotic) twins, but that’s strongly not recommended.”
#11: Fertility clinic success rates are not super important.
“Fertility clinic success rates are worth considering, but it could be hard to know a clinic’s success rates,” says Reed. “The truth is most IVF clinics have very comparable outcomes. We are all doing IVF in very similar ways. As of yet, nobody has some secret sauce that is making their treatment significantly more successful than the rest.”
What is important? “Finding a clinic that will treat you well,” says Reed. “Seek a doctor who makes you feel heard. A clinic that gives you the time of day and doesn’t make you feel like you’re being rushed through the process.”
More on Fertility:
- What It’s Really Like to Go Through IVF
- Making Sense of Secondary Infertility
- The Fertility Foods to Eat If You’re Trying to Conceive
- Advanced Maternal Age and Fertility
- How Infertility Impacts Your Mental Health
- After PCOS Led to Infertility, One Mom Found Solace in Others’ Stories
Disclaimer: The information on our site is NOT medical advice for any specific person or condition. It is only meant as general information. If you have any medical questions and concerns about your child or yourself, please contact your health provider.
SHARE THIS ARTICLE
MOST LOVED
Sleepytime Sidekicks












