BABY
Your Guide to Baby Ear Infections
More than 80% of children will have an ear infection before their third birthday. Here’s everything you need to know.

Written by
Happiest Baby Staff
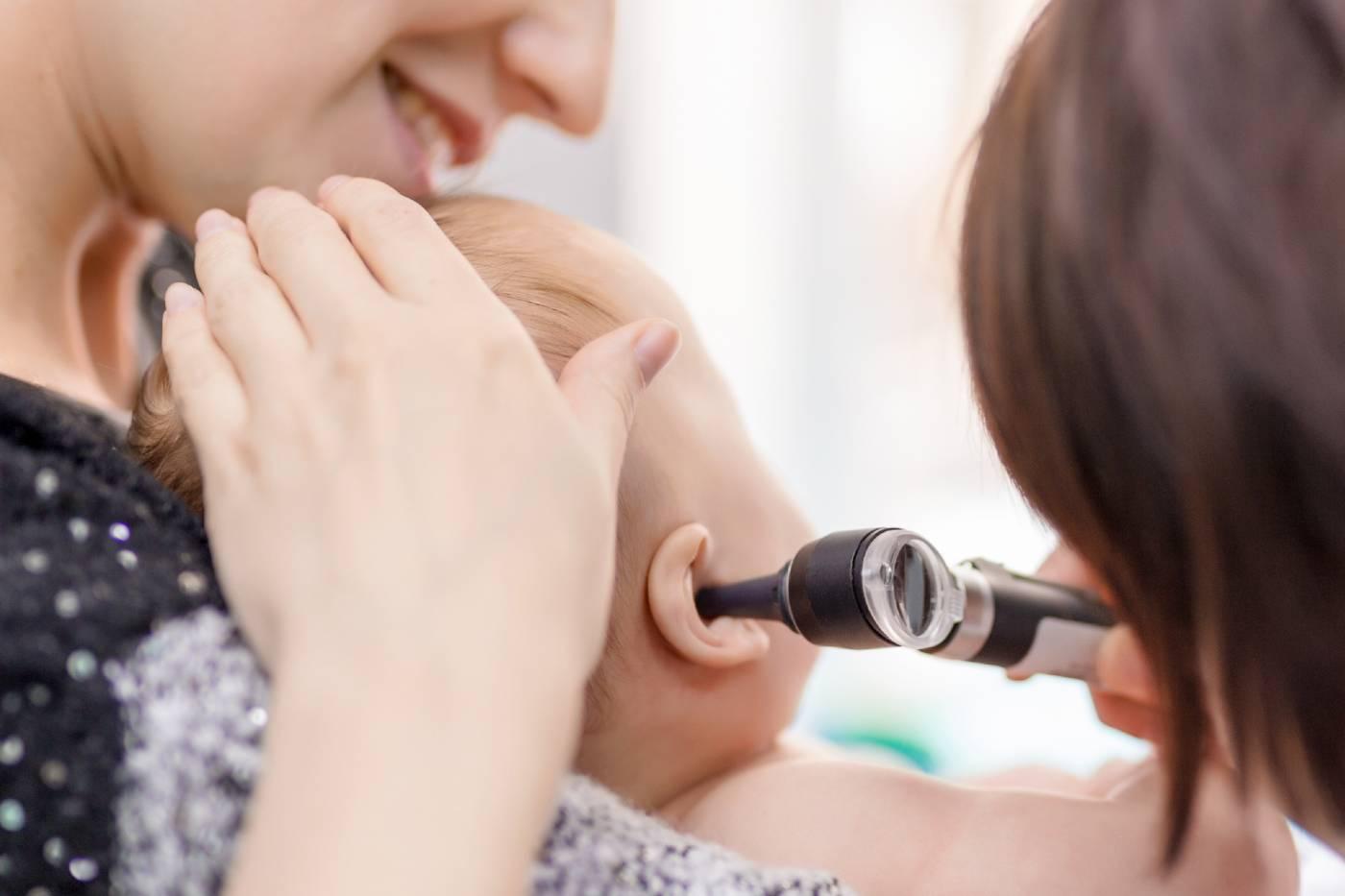
Here’s a familiar scene for parents: Your little one is tugging at their ears, fussing more than usual, and—uh-oh—does their forehead feel warm, too? There’s a good chance you’re dealing with the dreaded, yet oh-so common, ear infection. In fact, your first thought might even be, “ugh, here we go again!” So, what exactly is an ear infection—and can you prevent them? Here's all you need to know about ear infections in babies and toddlers.
Are there different types of ear infections in babies?
Ear infections are super prevalent in little ones, with five out of six children having at least one ear infection by the time they’re 3 years old. An ear infection, also known as otitis media, occurs when the middle ear becomes inflamed thanks to things like fluid buildup behind the eardrum. This can happen due to viral infections—the same ones that cause the common cold—or when the eustachian tubes, the narrow passageways that connect the middle ear to the back of the nose—become swollen. With that, not all ear infections are the same. Here’s the lowdown on the different types of ear infections:
- Acute otitis media: This is the most common type of ear infection. Here, fluid becomes trapped behind your tot’s middle ear, causing the eardrum to become swollen and infected.
- Otitis media with effusion: This occurs after an ear infection has already cleared, but the fluid lingers behind the eardrum.
- Chronic otitis media with effusion: Here, your baby no longer has an actual infection, but the fluid stays in the middle ear for a super long time or continues to come back again and again. This type of ear infection is more common in kiddos between 6 months and 3 years old and impacts more boys than girls.
- Otitis externa (aka Swimmer’s Ear): While other ear infections occur behind the eardrum, Swimmer’s ear happens when the outer ear canal becomes infected. (Swimming can cause water to get trapped, allowing bacteria to easily grow.)
What are the symptoms of an ear infection?
Since the tiniest tots can’t say “my ear hurts,” it can be hard to figure out when your baby has an ear infection. They might pull at their ears a lot…but this can also be their way of exploring or soothing themselves. Your baby might cry or be more fussy than usual, especially when being put down for a nap or nighty-night. They could also have a fever. At times, an ear infection can even impact your kiddo’s balance. Here are some common symptoms of an ear infection:
- Ear tugging
- Increased crying, especially when lying down
- Trouble sleeping
- Issues hearing
- Ear drainage
- Loss of appetite
- Pain
- Fever
- Headache
- Itchy, swollen, and/or red ears
- Loss of balance
Of note: With otitis media with effusion, your baby might not show any symptoms. However, delayed speech development could be a clue.
Why do children get so many ear infections?
Little ones are way more prone ear infections than grownups for a few reasons. For one, babies and kids are still developing…and so are their immune systems, making them more vulnerable to lots of icky illnesses. Also, the passages in their little ears are narrower and shorter than yours, making it easier for germs and fluid to get trapped in the middle ear and stay there. Adding to the issue: Children’s adenoids (tissue at the very back of one’s nasal passage) are pretty big, so they can interfere with the opening of eustachian tubes.
Can ear infections be prevented?
Not always! But there are a few things you can do to help reduce your sweetie’s risk of getting an ear infection. Like:
- Don’t smoke! Babies who are exposed to people who smoke tend to have more ear infections than those who live in smoke-free environments.
- Bottle-feed like this. Hold your nugget in an upright angle when bottle-feeding, so that Baby’s head is higher than their tummy. Horizontal feeding can cause fluid to flow back into the eustachian tubes. (Learn about paced bottle feeding.)
- Breastfeed if possible. The American Academy of Pediatrics (AAP) notes that infants who are breastfed for the first year are exposed to protective substances that help shield littles from bacterial and viral infections, like ear infections.
- Vaccinate! Keep your tyke up to date on their vaccinations, including the annual flu shot if your wee one is over 6 months old. (Research shows this helps!) It’s also super important to make sure your kiddo has received their pneumococcal vaccine, or PCV13, which has been shown to prevent ear infections. This is especially important for children in daycare.
- Keep colds at bay. Easier said than done, right?! But since most ear infections start with the common cold, do your best to avoid the seasonal sniffles with proper hand scrubbing; teaching your kiddo not to share toys, food, cups, and utensils with playmates; and staying away from friends who are under the weather.
- Dry off ears. To sidestep swimmer’s ear, dry off your tyke’s ears after swimming or bathing and leave your bub’s protective ear wax alone. You can also speak to your child’s doctor about trying swimmer's ear drops.
Do ear infections go away on their own?
Most ear infections do go away within two to three days without any treatment. However, babies who are under 6 months old almost always receive antibiotic treatment for ear infections. Part of the reason is that complications from ear infections can be significantly more severe when they occur in infants.
For children over 6 months old with mild to moderate ear infections, the decision to treat is one to be made between parents and their healthcare providers. Often, it’s best to simply watch and wait for two to three days, offering doc-approved OTC pain meds if needed. With that, wait-and-see might not be the ideal approach for children who have a cleft palate, Down syndrome, or another genetic condition, or children with an immune system disorder.
How are ear infections treated?
There are many reasons why antibiotic treatment for ear infections is no longer a knee-jerk go-to. For example, sometimes it's not clear what’s causing your child’s ear infection. And antibiotics only help bacterial ear infections. For this reason, your provider will likely have your kiddo wait a few days to see if symptoms get better on their own. (Again, this does not apply to babies under 6 months old and a few more exceptions mentioned above.) If there’s no change in your child’s symptoms in roughly two to three days, then antibiotic treatment may be an option.
The good news is: For the most part, antibiotics aren’t usually needed to treat ear infections, because the body’s immune system does a pretty great job of resolving them itself.
But if your child is prescribed antibiotics for their ear infection, it's important to make sure they get the full course of medication. Don’t stop just because your kiddo seems to be getting better. The infection may return if you halt treatment too soon. Equally important: Let your provider know if your baby doesn't seem to get better after a few days! Your nugget may need to try a different antibiotic.
Finally, if your child suffers from frequent ear infections (big hugs!), know that a new study in the New England Journal of Medicine suggests that a common treatment—placing tiny tubes in a child’s eardrum to help drain fluid—may not be an effective treatment for recurrent ear infections, after all. Instead, it seems babies and toddlers often grow out of the issue, whether they get tubes, antibiotics, or nothing.
More children's health need-to-know:
- Dr. Harvey Karp's Guide to Baby Constipation
- The Importance of the Flu Shot for Babies
- What to Expect at Well-Child Visits
- Keeping Baby's Teeth Healthy
****
REFRENCES
- National Institute on Deafness and Other Communication Disorders. Ear Infections in Children
- Children’s Hospital of Philadelphia. Otitis Media with Effusion (OME)
- Centers for Disease Control and Prevention (CDC): Ear Infections
- American Academy of Pediatrics (AAP). Ear Infection Information
- Nemours Children’s Health, KidsHealth. Middle Ear Infections (Ottis Media)
- Acute Otitis Media and Other Complications of Viral Respiratory Infection. April 2016
- AAP: Swimmer’s Ear in Children
- AAP: Middle Ear Infections
- Tympanostomy Tubes or Medical Management for Recurrent Acute Otitis Media. New England Journal of Medicine. May 2021
Disclaimer: The information on our site is NOT medical advice for any specific person or condition. It is only meant as general information. If you have any medical questions and concerns about your child or yourself, please contact your health provider.
SHARE THIS ARTICLE
MOST LOVED
Sleepytime Sidekicks












