BABY
Jaundice in Newborns: Everything You Need to Know
Don’t let this common newborn condition take you by surprise!

Written by
Happiest Baby Staff
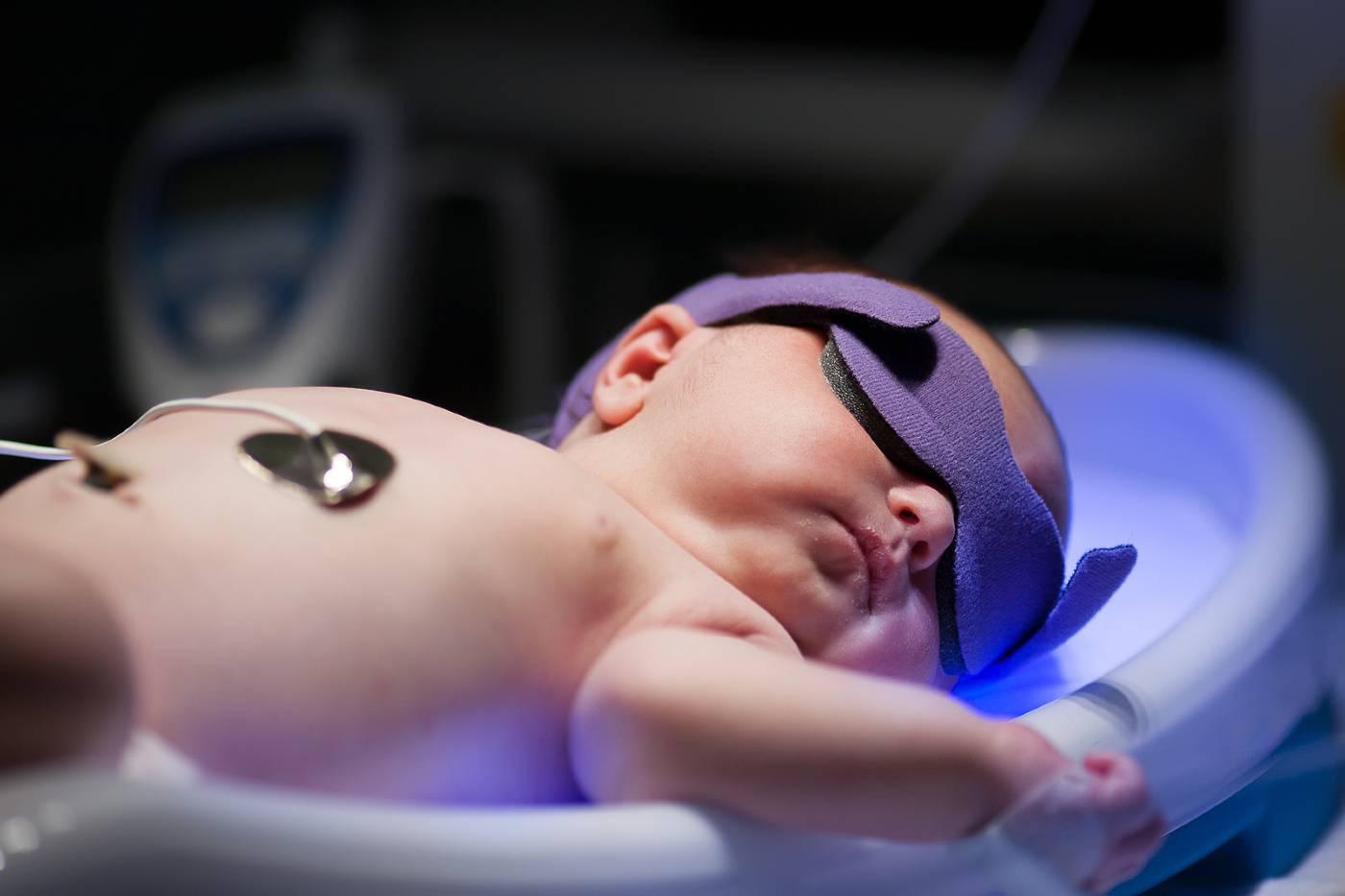
While it’s pretty darn common for babies to develop the yellowish hue of jaundice in the days after birth, many new parents are startled and worried by this sudden change in color. But is newborn jaundice really something to worry about? Before you start to panic, let’s break down the signs, symptoms, and treatment of jaundice—and suss out when concern is warranted. Plus, learn if it’s possible to prevent your baby from getting jaundice in the first place.
What is jaundice?
Newborn jaundice (aka hyperbilirubinemia) is when your baby’s skin (and sometimes eyes) appears yellow. The yellow hue is the result of excess bilirubin in your little one’s system. Bilirubin is the natural result of red blood cells breaking down. It’s a substance that’s present in everyone’s blood, but a newborn’s liver is usually not mature enough to efficiently remove it from their body. That’s why up to 60% of all full-term—and up to 80% of premature—babies develop jaundice during their first week of life. It’s so common, in fact, that newborn jaundice is actually considered a “normal part of the newborn period.” The condition usually peaks during a baby’s first two to five days of life and lasts about one to two weeks—but can stick around longer for breastfed babies.
What causes jaundice in newborns?
Bilirubin buildup leads to jaundice. During pregnancy, Mom’s liver took care of removing Baby’s bilirubin. But after birth, that task moves to your newborn’s to-do list and, according to the American Academy of Pediatrics (AAP), it takes a few days for a baby’s liver to effectively get the job done. That lag time coupled with the fact that babies have more red blood cells than older children and those cells don’t last very long, means newborns experience a lot of cell breakdown and a lot of bilirubin buildup. The resulting jaundice is called physiologic jaundice, which is the most common type of newborn jaundice.
Does breastfeeding cause jaundice?
It’s true that jaundice is more common in babies who are breastfed than babies who are formula-fed, but that in no way should discourage you from nursing! Jaundice related to breastfeeding is only temporary. Here’s what you need to know about breastfeeding and jaundice:
-
Breastfeeding jaundice: Breastfeeding jaundice occurs when your little one doesn’t get enough breastmilk. That lack of milk then leads to less movement in the gut and less bilirubin elimination. This can happen if your breastmilk hasn’t come in yet or if you’re experiencing nursing difficulties. (Breastfeeding your baby at least 8 to 12 times a day for the first few days will improve your milk supply and help keep your baby’s bilirubin level down.) - Breastmilk jaundice: Here, breastmilk itself can negatively affect how your newborn’s liver breaks down bilirubin, leading to a buildup of the substance. Breastmilk jaundice occurs late in the first week, peaks during the second week, and usually resolves by the time your baby is two weeks old. It occurs in about 2% of babies.
Other Jaundice Causes
At times, a medical problem or underlying condition causes newborn jaundice. In these cases, jaundice often appears much earlier or much later than more common types of infant jaundice. Underlying conditions that can lead to newborn jaundice include…
-
ABO or Rh Incompatibility: A small number of babies have a different blood type than their birthing parent, which can lead to quick breakdown of red blood cells. (You should’ve had an antibody screening during your first trimester and possibly a repeat test at 28 weeks to help determine if this might be an issue.) - Genetic Condition: When a newborn has a G6PD deficiency, their body doesn’t produce enough of an enzyme that ensures their red blood cells work correctly. Research shows that 13% of Black boys and about 4% of Black girls have G6PD deficiency. Other genetic conditions that lead to jaundice include Gilbert syndrome and Crigler-Najjar syndrome.
- Poor Liver Function: An infection or a condition like hepatitis or cystic fibrosis can negatively affect liver function and lead to jaundice.
- Biliary Atresia: This is a condition in which a baby’s bile ducts are blocked or scarred.
What babies are at a higher risk of jaundice?
While jaundice is very common among newborns, some babies are at a greater risk for high levels of bilirubin than others. If your newborn falls into any of these buckets, the AAP suggests you ask your doctor about an early jaundice follow-up:
- Your baby was born more than two weeks early (before 37 weeks).
- A parent or sibling experienced high bilirubin levels after birth that required light therapy.
- Breastfeeding is not going well.
- Your newborn experienced bleeding under the scalp due to a difficult delivery.
- Your baby has a lot of bruising related to labor and delivery.
- Your baby is of East Asian or Mediterranean descent.
- Your baby has Down syndrome.
- Your baby weighed 9 to 10 pounds at birth—and their birthing parent is diabetic.
It’s also important to schedule an early follow-up appointment if your little one was flagged for jaundice in the first 24 hours after birth and/or has a high bilirubin level before leaving the hospital.
Signs Your Baby Has Jaundice
The biggest telltale of newborn jaundice is the appearance of yellow skin. The whites of your baby’s eyes may become yellow, too. Jaundice usually first appears on a baby’s face, then the yellowing migrates to the chest, tummy, arms, and legs as bilirubin levels increase in the body. The AAP notes that the best way to see jaundice is in the daylight or under fluorescent lights. If you still can’t tell if your baby’s jaundice, gently press on a spot on your baby’s skin that’s close to the bone, like their forehead, nose, chest, or shin. If your baby has jaundice, their skin will appear yellow when you lift your finger.
It’s important to note that it can be more difficult to spot jaundice in babies with dark skin. If you’re unsure if your darker skin baby has jaundice, check their eyes, palms, and soles for yellowing, as well as under their tongue.
Beyond skin color, dark urine and pale stool are common symptoms of jaundice. Normal newborn urine is either colorless or light yellow and healthy newborn stool is yellow, orange, green, or brown, not gray, beige, white, or otherwise pale.
How is jaundice diagnosed?
All babies are screened for jaundice via a blood test or a skin test, which uses a special light to measure bilirubin in the skin, before leaving the hospital or birth center. If your newborn appears to be jaundiced within their first 24 hours of life, their bilirubin levels will be measured ASAP.
Your baby should be checked for jaundice once again during their first visit to the doctor. (If your baby was discharged before 48 hours, they should be seen within two days for another screening.) Whether your little one requires even more bilirubin screening depends on their age, the level of bilirubin initially measured, and whether your bub is at an elevated risk for jaundice.
How is newborn jaundice treated?
Good news! Most cases of newborn jaundice require zero treatment. When treatment is needed, however, here’s what’s used:
-
Phototherapy: For this jaundice treatment, your undressed but diapered newborn is either placed under special blue lights (“bili lights”) designed to help lower the level of bilirubin in their body—or they’re wrapped in a blanket fitted with the same type of lights (this is called fiberoptic phototherapy). Your baby will wear special shades to protect their eyes. Phototherapy jaundice treatment is usually done in the hospital, but at times can be done at home. This is the most common treatment for newborn jaundice and generally takes one to two days. - Frequent feeding: Offer 10 to 12 feeds a day to help your baby poop and pee more, which’ll help get rid of bilirubin. (Babies should produce at least six wet diapers over a 24-hour period.)
- Supplementation: If your baby’s jaundice is related to breastfeeding, your physician may suggest supplementing breastmilk with infant formula to help lower bilirubin levels.
- IV Fluids: In rare cases, a newborn may receive extra fluids by IV to help treat jaundice.
- Transfusion: In extremely rare cases when other jaundice treatments don’t work, your healthcare provider may recommend something called an exchange transfusion where some of your little one’s blood is replaced with fresh, donated blood.
Can you prevent jaundice?
While there’s no way to completely prevent newborn jaundice, there are things you can do to diminish the impact, such as…
-
Avoid these foods and products. Let your healthcare provider know if you eat fava beans or if you use mothballs, antibiotics, henna, or any herbal remedies. While rare, all of these items have been shown to cause severe jaundice. - Get your bloodwork done. It’s important that your blood type and antibodies are checked during pregnancy. If you’re Rh negative or if you have type O positive blood, follow-up testing on your infant’s cord is recommended.
- Visit a lactation consultant. This type of nursing expert can help improve your newborn’s latch and offer helpful advice for boosting your little one’s breastmilk intake. When babies don’t get enough to eat in their first three to five days, they have a higher risk of jaundice.
- Ask for written info. Before getting discharged from the hospital or birth center, you should get written information about jaundice, your newborn’s bilirubin level, and other lab tests—plus, clear instructions about when your little one needs to see the pediatrician next.
- Keep follow-up appointments. Skin color alone is not a good way to tell if your newborn’s jaundice is getting worse! That means, always keep your follow-up appointments, and have any tests done that your pediatrician recommends.
Is jaundice dangerous?
Most of the time, babies have mild cases of jaundice that are considered harmless. In rare cases, affecting far less than 1% of infants, bilirubin levels can get exceedingly high and cause brain damage (kernicterus) leading to complications such as cerebral palsy or deafness. If a newborn has very high bilirubin levels, it’s considered a medical emergency that requires admission to the intensive care unit, where they’ll receive an exchange transfusion to rapidly decrease their bilirubin levels. To sidestep an emergency, it’s important to reach out to your healthcare provider if you notice any of these symptoms in your newborn:
-
Skin is becoming increasingly yellow - The yellow hue has progressed to your baby’s tummy, arms, or legs
- Baby’s eyes are now yellow, too
- Very sleepy
- Increasingly fussy and hard to console
- Not nursing or taking infant formula well
- Has not wet at least six diapers in 24-hour period
- Fever
- Frequent vomiting
- Jaundiced for more than two weeks if formula-fed
- Jaundiced for more than four weeks if primarily breastfed
Call 911 or head to the ER if your baby exhibits the following symptoms:
-
Backward arching neck or body - Trouble waking up
- High-pitched cry
- Inconsolable crying
- Strange eye movements, such as gazing upward
More Newborn Need-to-Knows:
- Dr. Harvey Karp’s Expert Newborn Sleep Tips
- Newborn Circumcision Care 101
- The 411 on Newborn Screenings
- Newborn White Noise Benefits
- Learn The 5 S’s For Soothing Newborns
- How to Dress Your Newborn
- Your Newborn’s First Poop, Explained
***
REFERENCES
- Cleveland Clinic: Jaundice in Newborns
- Harvard Health Publishing, Harvard Medical School: New guidelines on newborn jaundice: What parents need to know
- American Academy of Pediatrics (AAP): Jaundice in Newborns: Parent FAQs
- March of Dimes: Newborn jaundice
- The Nemours Foundation, KidsHealth: Jaundice in Newborns
- Neonatal Jaundice. StatPearls. February 2023
- Boston Children’s Hospital: Hyperbilirubinemia and Jaundice
- Mayo Clinic: Infant jaundice
- The American College of Obstetricians and Gynecologist (ACOG): The Rh Factor: How It Can Affect Your Pregnancy
- Clinical Practice Guideline Revision: Management of Hyperbilirubinemia in the Newborn Infant 35 or More Weeks of Gestation. Pediatrics. September 2022
- Nationwide Children’s: Jaundice in Children
- National Health Service (NHS): Newborn jaundice
- MedlinePlus: Newborn jaundice
Disclaimer: The information on our site is NOT medical advice for any specific person or condition. It is only meant as general information. If you have any medical questions and concerns about your child or yourself, please contact your health provider.
SHARE THIS ARTICLE
MOST LOVED
Sleepytime Sidekicks












